A history of structural racism and implicit bias coupled with unmet socioeconomic needs has created a Black maternal health crisis in the United States, with Black birthing people facing the highest rates of maternal mortality in the country. A 2021 Centers for Disease Control and Prevention report indicated that Black birthing people are three times more likely to die during childbirth than white birthing people.
By integrating social care into health care, essential hospitals can play a pivotal role in combating the underlying social inequities that contribute to poor obstetric outcomes for Black birthing patients.
This blog is intended as a guide to demonstrate how essential hospitals can build strong social support programs to help improve Black obstetric outcomes. While there are many strategic frameworks to address social integration of care, this blog highlights one hospitals can use to achieve significant changes.
Framework
A 2019 National Academies of Sciences, Engineering, and Medicine (NASEM) report analyzed approaches to integrate social care into health care and offered evidence-based recommendations through a five-step framework focused on awareness, adjustment, assistance, alignment, and advocacy (see Figure 1). Using this framework, essential hospitals can assess patients’ needs through screening for social needs, adjust clinical care to acknowledge social barriers, assist patients, align with community needs, and advocate for larger structural changes.
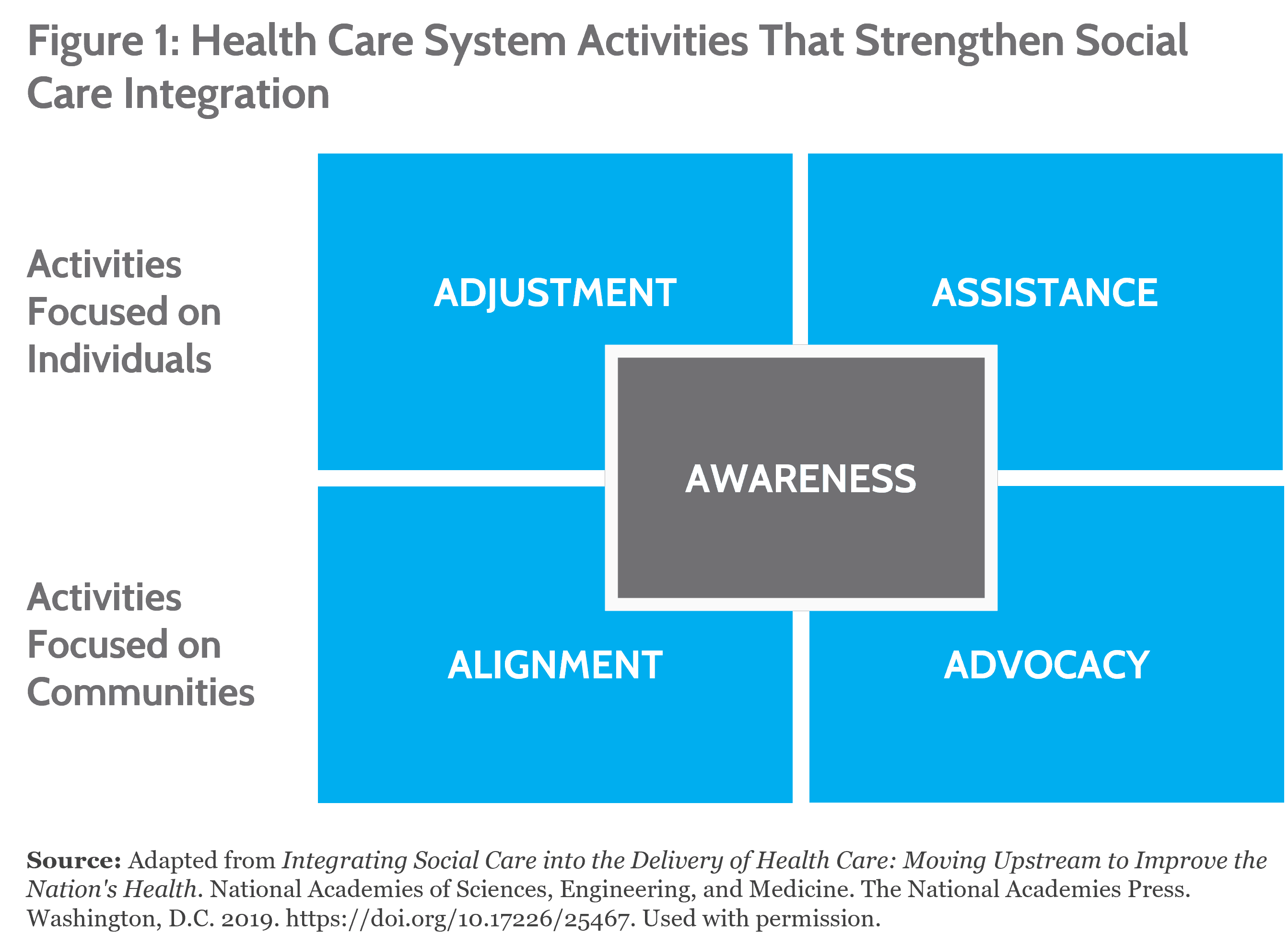
Awareness
During the awareness stage, hospitals assess the social needs of their patient populations, typically through a screening process to identify social factors that contribute to a patient’s health outcomes. Screening tools are extremely effective when distributed to patients in emergency departments and primary care settings. It is a valuable tool to learn about patients’ complex needs.
Boston Medical Center (BMC), in Boston, pioneered a screening tool, THRIVE, to assess patient needs. THRIVE is a health-related social needs assessment tool composed of several questions that allow providers to match patients with resources based on their needs, such as housing and food resources. Patients complete the screening at every visit, and their results are reviewed and notated in their charts. Those who indicate facing barriers that affect their clinical care are connected to other resources and in-house programs that provide additional support. BMC’s THRIVE team is excitedly working on THRIVE 2.0 to revamp the screening tool and digitize the platform for easier patient access.
Adjustment
The next step is adjustment of clinical care by incorporating a patient’s social needs into clinical decision-making. Adjustments can vary from providing interpreter services to overcome language barriers to offering after-hours appointments to accommodate working patients.
BMC mitigates hypertension in birthing patients with an innovative remote blood pressure system to identify patients at risk of preeclampsia and monitor birthing patients with a hypertensive condition. BMC gives blood pressure cuffs to any patient who meets U.S. Preventive Services Task Force criteria for being at risk of preeclampsia and trains patients via telehealth to use the cuffs and understand results. The blood pressure machine is an advanced, cellular-enabled device that doesn’t require a cellphone or internet access, allowing patients to easily manage their care. The readings automatically transmit directly into a patients’ electronic health record. The program has opened the opportunity for providers to treat patients with undiagnosed hypertension earlier in pregnancy. Collaboration between the clinical team and the operations staff is essential to the program’s success and has improved patients’ ability to receive attentive, quality care.
Assistance
Assistance encourages health systems to connect patients with relevant community, public, and government resources, as needed. Interventions in this category can be lighter touch or intensive. Lighter touch interventions typically are one-time provisions, such as providing referrals, resources, or other information. For example, hospitals can refer birthing patients facing food insecurity to no-cost community food pantries. Intensive interventions assess patient social needs more comprehensively and typically are directed to medically and socially complex patients.
NYC Health + Hospitals, in New York, created the Maternal Medical Home with support from city hall to address maternal health disparities in New York City. The program uses maternal care coordinators and social workers to provide relevant services to patients through referrals. Providers identify patients’ needs with screenings for social health, behavioral health, and complex clinical needs. The program links patients with a multitude of community resources available through the state’s health department, including nonclinical birth worker support and home visits for newborns. Community resources are accessible to all 11 acute-care facilities in the health system. Since 2019, the program has had more than 5,000 unique patients and more than 14,000 referrals. Wendy Wilcox, MD, MPH, MBA, chief women’s officer of NYC Health + Hospitals, believes the maternal medical home is just one way NYC Health + Hospitals provides integrated care to patients and their families.
Alignment
Alignment and advocacy, which go hand-in-hand, are the final two steps in the framework. Alignment stresses the importance of investing and deploying community social care assets, such as community leaders and organizations, to improve health outcomes. Hospitals can engage in cross-sectoral coalitions, such as medical-legal partnerships, to assist patients. Also, health systems can partner with social care agencies to provide services, such as home-delivered meals and case management.
Memorial Healthcare System, in Hollywood, Fla., formed community partnerships to create the Mothers Overcoming Maternal Stress (MOMS) Program. Memorial Healthcare has provided case management services to its patients for more than 25 years, but the MOMS program extends beyond typical services, combining case management with parent education and social support. The program offers services, such as food delivery, emergency funding, and daycare enrollment assistance.
Tim Curtin, MSW, MBA, the system’s executive director of community services, attributes much of the program’s success to Memorial Healthcare’s active community engagement through partnerships with local nonprofits, faith-based organizations, and other community pillars. Gloria Villalobos, M. Ed., team leader of the MOMS program, finds value in using community spaces for programming, such as yoga instruction, to provide patients with safe, familiar spaces to help build trust. The program staff creates a supportive environment for their patients to ensure they can sustain healthy lives beyond the hospital walls.
Advocacy
Through advocacy, health care organizations promote policies that address health and social needs and strengthen their communities. One of the most effective advocacy tools is developing an anchor strategy. Anchor institutions are universities, hospitals, and other large organizations that play a pivotal role in the economic development of local communities. As community pillars, essential hospitals have the power to implement large-scale change on the local, state, and federal levels.
Denver Health, in Denver, is an anchor institution with a mission to advance health equity for its patients, staff, and community members. Through its Office of Health Equity, established in 2022, Denver Health launched several initiatives to support its goals of improving health outcomes, life expectancy, and quality of life for patients in its community. Identifying areas of increased health disparities helped Denver Health create programs that prioritize patients facing barriers to equity and opportunity, such as a maternal health equity group focused on maximizing access to prenatal care to detect and treat high-risk conditions.
Denver Health also recognizes the opportunity to grow alongside its community and promotes community development through partnerships with local public schools to create pipeline programs and a workforce development center offering skills training for career advancement. Building community partnerships, addressing community priorities, and working to eliminate socioeconomic barriers in the community are priorities at the forefront of Denver Health’s work. The health system continues to find ways to merge clinical and social work to ensure its patients can have unrestricted access to quality care, all while investing in and prioritizing the development of the community it has served for more than 160 years.
Recognizing the unique needs of its members, America’s Essential Hospitals advocates at the federal level on the most pressing issues affecting essential hospitals, including Black obstetric outcomes. The association proudly supports the reintroduction of the Black Maternal Health Momnibus Act and endorses the legislation. Association members are encouraged to read the association’s weekly legislative digest, On the Hill, to stay up to date with legislative developments.
Conclusion
Black birthing patients are one of the most vulnerable populations in the country. It is imperative that all facets of health systems prioritize the improvement of Black obstetric outcomes and reduce the alarming maternal mortality rates. Essential hospitals have a unique role in this mission because of the patient populations they serve, and centering Black birthing patients in health equity efforts, creating programs, and deploying community resources can remedy social factors that affect these outcomes.
Thank you to our members Boston Medical Center, NYC Health + Hospitals, Memorial Health, and Denver Health for their contributions to this blog. Also, thanks to the advocacy team at America’s Essential Hospitals for their diligent advocacy efforts, especially regarding maternal health.